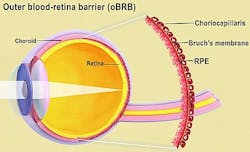
Scientists used patient stem cells and 3D bioprinting to produce eye tissue that will advance understanding of the mechanisms of blinding diseases. The research team from the National Eye Institute (NEI), part of the National Institutes of Health, printed a combination of cells that form the outer blood-retina barrier—eye tissue that supports the retina's light-sensing photoreceptors. The technique provides a theoretically unlimited supply of patient-derived tissue to study degenerative retinal diseases such as age-related macular degeneration (AMD).
Researchers combined three immature choroidal cell types in a hydrogel: pericytes and endothelial cells, which are key components of capillaries; and fibroblasts, which give tissues structure. The scientists then printed the gel on a biodegradable scaffold. Within days, the cells began to mature into a dense capillary network.
On day nine, the scientists seeded retinal pigment epithelial cells on the flip side of the scaffold. The printed tissue reached full maturity on day 42. Tissue analyses and genetic and functional testing showed that the printed tissue looked and behaved similarly to native outer blood-retina barrier. Under induced stress, printed tissue exhibited patterns of early AMD such as drusen deposits underneath the RPE and progression to late dry stage AMD, where tissue degradation was observed. Low oxygen induced wet AMD-like appearance, with hyperproliferation of choroidal vessels that migrated into the sub-RPE zone. Anti-VEGF drugs, used to treat AMD suppressed this vessel overgrowth and migration and restored tissue morphology.